Introduction to RHN therapy services
Introduction to RHN therapy services
We offer several therapies to support patients and residents which ensure their needs are met, in a tailored and individual way. The therapy teams at the RHN ensure all patients and residents can fulfil their full potential and reduce the long-term complications of neuro-disability. The therapists work closely with the whole multidisciplinary team to ensure the delivery of a holistic service.
The hospital is split between two main services. The first is the brain injury service for people who need complex rehabilitation or for those with prolonged disorders of consciousness. The second is a specialist nursing home for people with physical disabilities and cognitive behavioural needs.
We have 120 Allied Health Professionals.
What each therapy group does at the RHN
Physiotherapy
We have a large physiotherapy department that works across continuing care, specialist services and BIS at the RHN. Physiotherapists work within a multidisciplinary team to help a patient set goals relating to their current and predicted physical abilities. They assess the components of movement (muscle strength, joint range, sensation, coordination and balance) and determine how these affect an individual’s ability to achieve their goals, live and be independent within their environment.
Physiotherapists support patients and their families as they plan for the future. Physiotherapists use a broad range of skills and knowledge to create an individualised treatment plan. Treatments may occur in 1:1 sessions on a ward, in a gym, in a group or out and about on the RHN grounds and local community. Treatment is specific to the patient and based on current evidence-informed practice.
We have 30 permanent team members across the RHN.
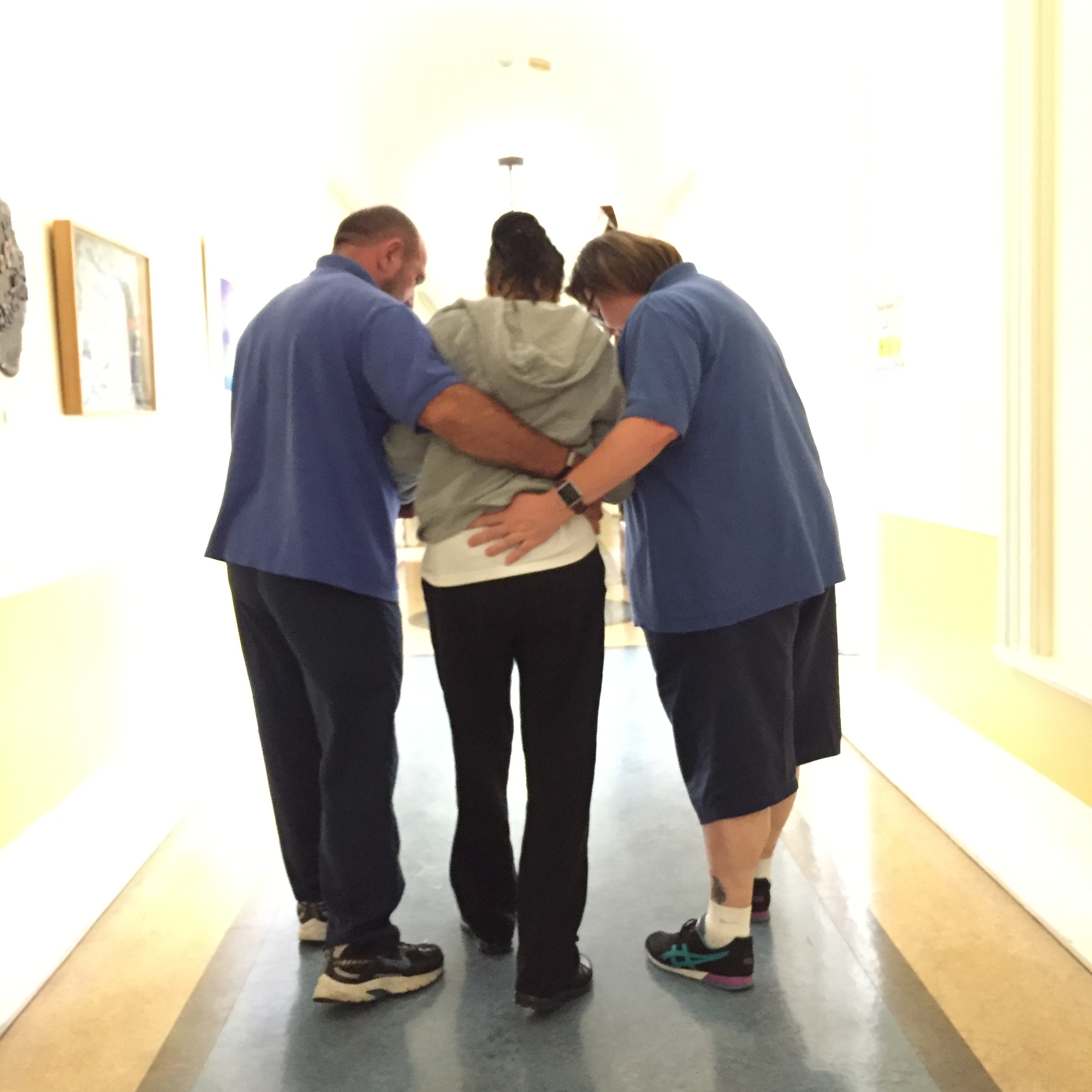

‘Over the years I worked with so many wonderful people from all over the world, which has been very inspirational. We have a very holistic approach as patients are here for longer periods, which allows you to really get to know the patients and their families. There is so much expertise under one roof and I do feel we achieve things here that could not have been quite so well elsewhere’. (Kristian Pallesen, Senior 1 Physiotherapist)
‘I have worked here for over 20 years and have seen many changes, such as the gyms changing! I have stayed at the hospital because it is like a family, and it has always felt like a close family as you get to know most of the staff and patients and everyone seems to know someone who worked here. My parents and brother worked here for many years. It is a lovely place to work and we have amazing grounds that are amazing for the residents. (Lisa Sewell, Physiotherapy Technical Instructor)
Occupational therapy
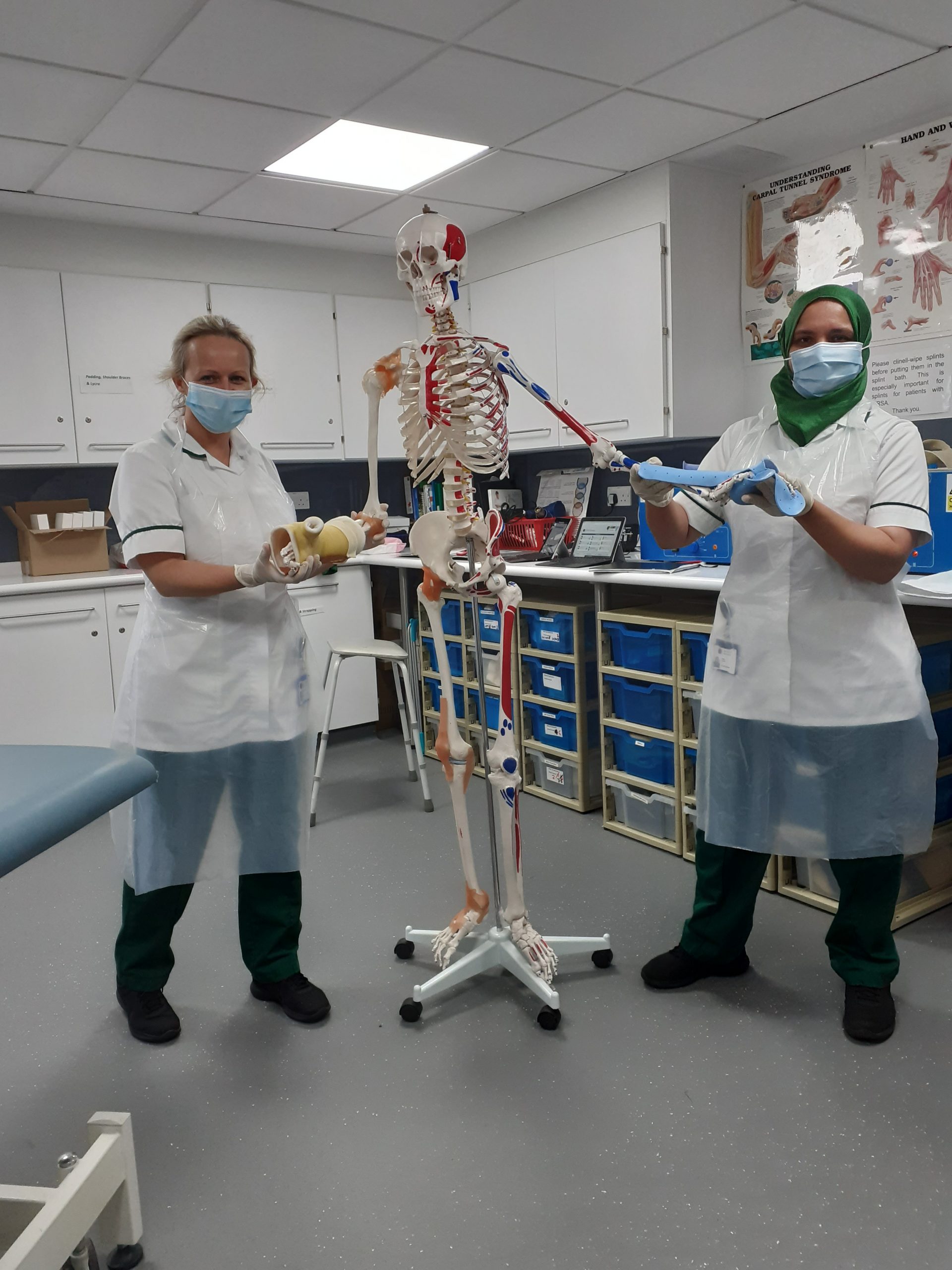
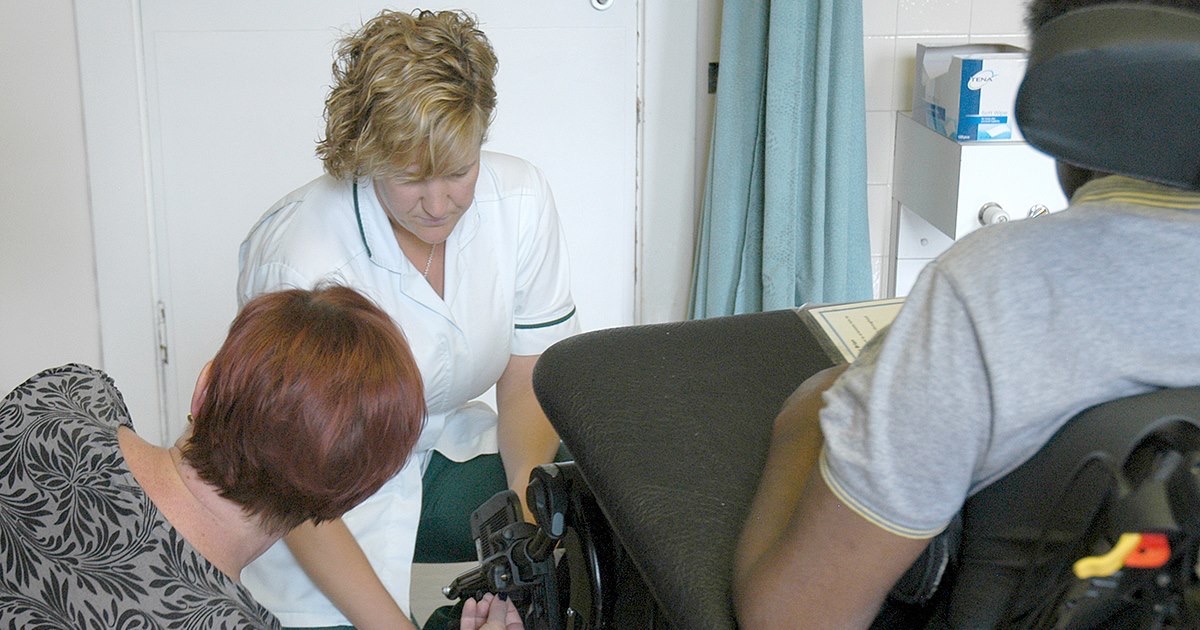
Occupational therapists (OTs) provide practical support to our patients and residents to try to overcome the barriers preventing them from doing the activities (or occupations) that matter to them. This may include activities such as preparing a meal, getting washed and dressed or leisure activities.
Occupational therapists can use equipment (such as splints) and teach different methods to find alternative ways of doing the activities which are more difficult because of the challenges of illness or disability.
We have 29 staff members that work on the OT team.

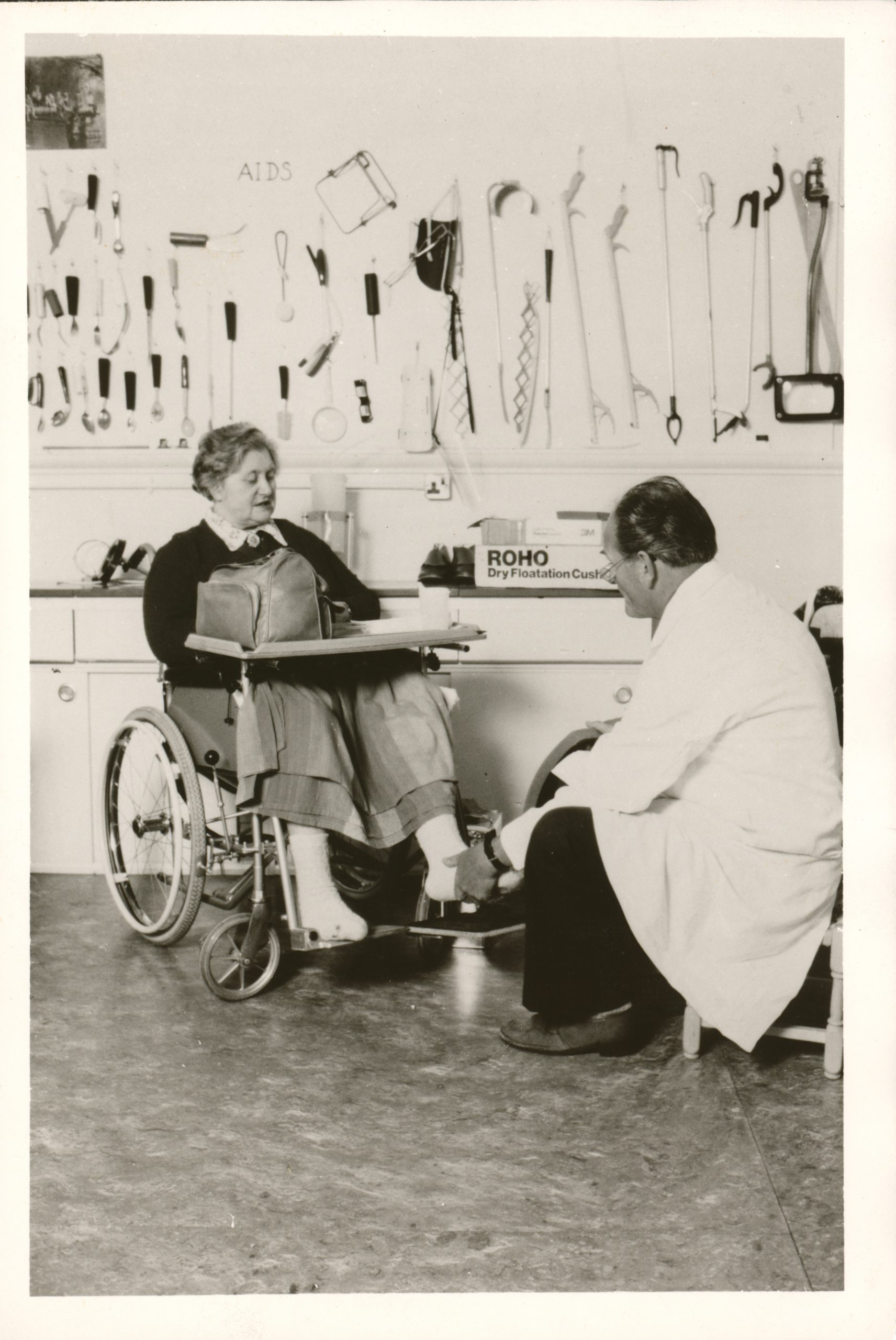
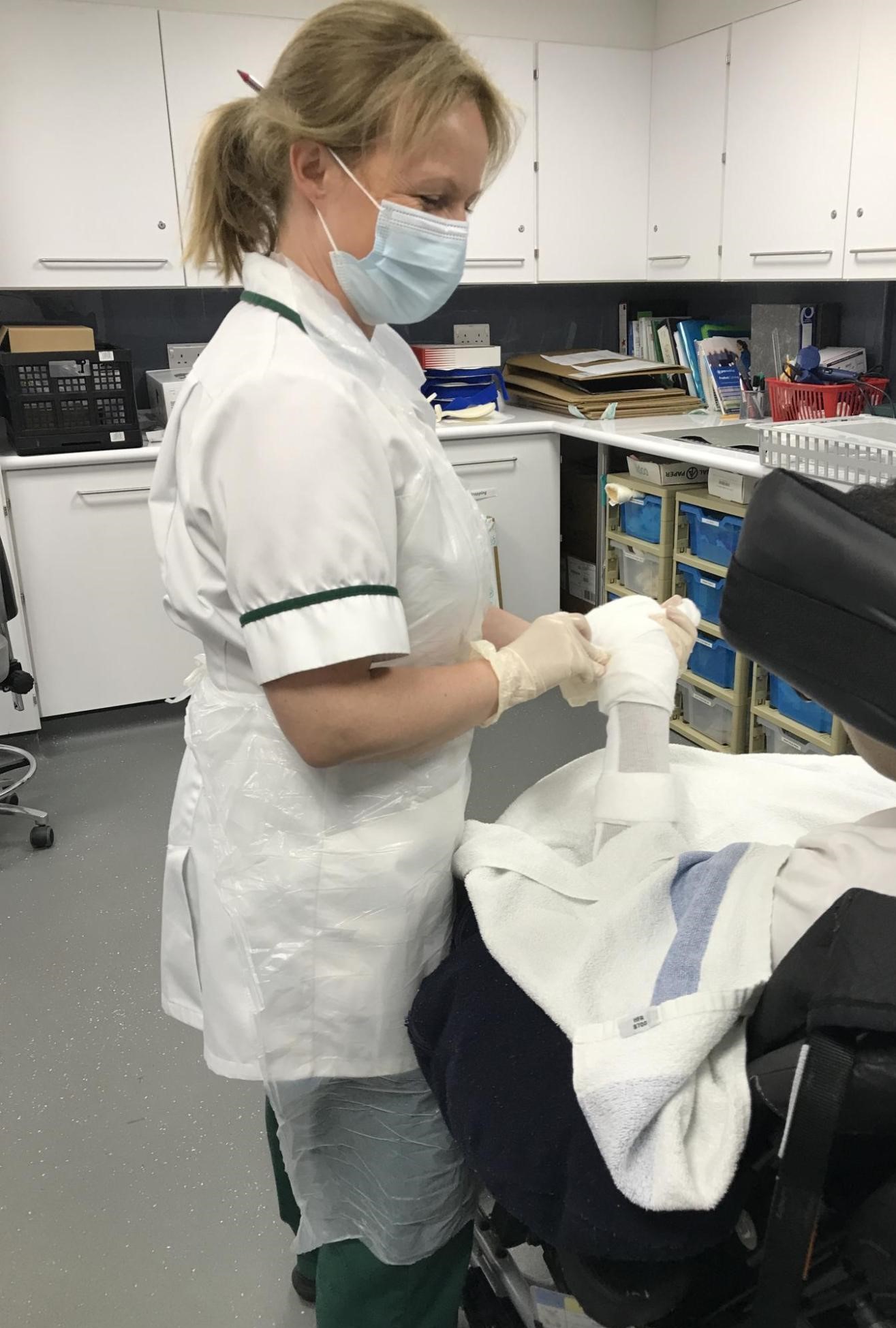
‘I have worked at Putney for a long time and what keeps me here is the sense of community. There is a common goal among the staff, families and volunteers to make the lives of patients and families as full and enriched as possible. I always say that if someone I loved had a brain injury, I would want them to come to Putney. I know they would be well cared for because the therapy and ward staff always go the extra mile and offer the best they can at the most difficult time in the lives of our patients and those who love them (Dani, OT lead).’







Speech and language therapy
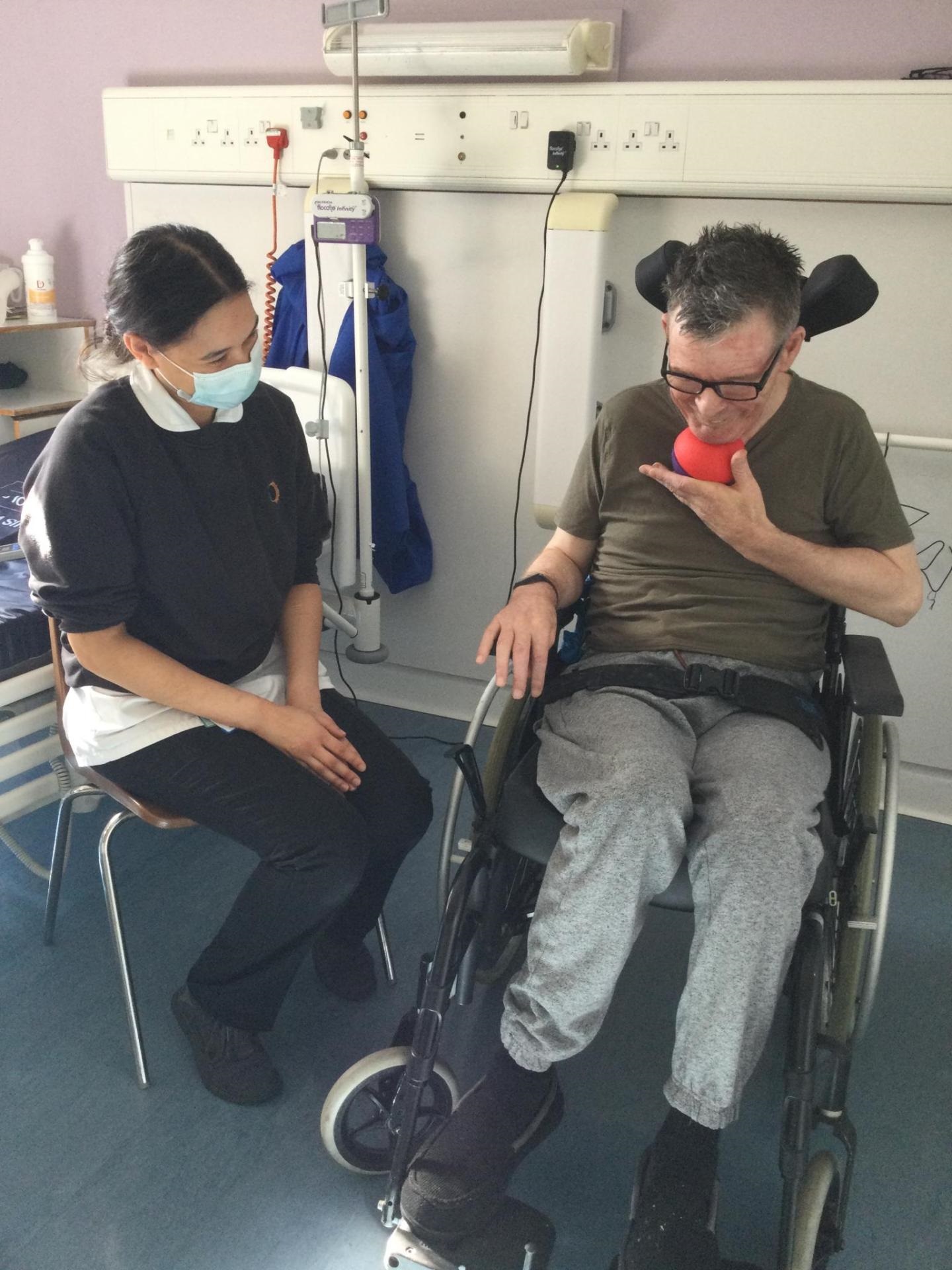
Speech and Language Therapists (SLTs) provide assessment, therapy and management of swallowing and communication difficulties. SLTs help our patients to communicate via whatever means they can – which may include speech, non-verbal communication (such as gestures, writing, and facial expressions), using picture-based communication charts, or high-tech means such as iPads or eye gaze-controlled devices. They support patients to express their needs, wants, wishes and choices as far as possible.
SLTs also help with safe eating and drinking if a person has problems swallowing. This may involve changing the consistency of food/fluids or providing exercises or strategies to help. SLTs also support people who have difficulties in swallowing their saliva and with weaning from tracheostomy tubes. All patients have access to specialist instrumental swallow assessments to help guide their management where needed.
[/panel]
Music Therapy
Music therapy is a clinical intervention, delivered by Health and Care Professions Council (HCPC) registered music therapists. Within neuro-rehab settings, music therapy is used to support rehabilitation in areas such as communication, mobility, cognition and emotional well-being. Methods employed include instrumental improvisation, songwriting, song singing and specific neurologic music therapy techniques.
At the RHN there are 5 music therapists and a music therapy assistant. We run groups, individual sessions and joint sessions with other disciplines.

Dietetics
Dietitians are qualified and regulated health professionals that assess, diagnose and treat dietary and nutritional problems at an individual and wider public-health level. They use the most up-to-date public health and scientific research on food, health and disease which they translate into practical guidance to enable people to make appropriate lifestyle and food choices.
The dietitians at the RHN are responsible for making sure that each patient’s nutritional needs are met. Following a brain injury, many patients have difficulty swallowing and may rely on tube feeding to receive all of their nutrition and hydration.
Some may have a combination of tube feeding and food by mouth due to difficulties in taking in enough food. Others may be able to fully eat and drink by mouth but require additional help to maintain a healthy weight.
Our dietitians monitor every resident and patient’s weight and adjust nutritional guidelines according to their individual needs.
We have 6 dietitians that work across RHN
‘Working as a dietitian at the RHN, I enjoy being able to make a difference to the patients and residents under my care. Being able to positively influence the nutritional status of so many individuals whilst working within a very caring and professional multi-disciplinary team, I find my working life at the RHN to be very rewarding. The ward team’s delivery of kind and compassionate care to their patients and residents is so refreshing to see and makes the RHN a place I would recommend to work at as well as for those that seek exceptional care’ (Emma Craig, clinical Lead Dietitian)
Social Work
The social work department has a number of tasks which include however is not limited to – providing practical and emotional support to patients and loved ones, chairing several different meetings, facilitating discharges and care packages alongside the MDT, and being the link between the hospital and community, advocating for public funds for patients and families, empowering and enabling patients to have an opportunity to be heard.
Clinical Psychology
The RHN Clinical Psychology team are a group of fully trained and registered mental health and neuropsychology professionals. The team currently consists of two consultant psychologists, two principal clinical psychologists, six clinical psychologists and two assistant psychologists, as well as trainees and honorary assistant psychologists that work at the RHN as part of their training.
In a neuro-rehabilitation setting, clinical psychologists assess cognition, mood, behaviour, and complex mental capacity decisions and create intervention plans for all of these to suit patients’ needs. This is completed using formal assessments, observations in sessions, group sessions and one-on-one talking sessions. Alongside this, the psychology team provide psycho-education on brain injury to patients, families and staff. We work closely with lots of different members of the multi-disciplinary team to create a formulation to understand each patient and how best to help them.
The RHN psychology team also supports families and staff with their well-being, provides various training sessions internally and externally, and is passionate about promoting ongoing research and development at the RHN.


‘I have been at Putney for 5 years now. I worked here initially as a locum for 6 months. I then returned as soon as a full-time post was available. I love the team spirit at the RHN. I also feel that the focus on the whole person and seeing each patient and resident for who they are as individuals are unique and special. The RHN has supported me to progress in my career by offering me opportunities to study, and now I am an RHN PhD fellow. I would not get these opportunities elsewhere. The people at the RHN and the care and therapy I see every day make me proud to work at Putney. (Alex, Principal Clinical Psychologist)’
Leisure and Family services
Our Leisure and Family Services (LaFS) team provides and coordinates a wide range of social and leisure activities for our patients and residents, both on the wards and the wider hospital grounds. The team includes a dedicated group of volunteers who bring a wide range of skills and experience, providing companionship and practical support for patients in a variety of activities
OT Art service
The occupational therapy art room is a creative space used by patients and residents across the entire hospital.
The art service is accessed via a referral through a patient’s Occupational Therapist. Often patients come to the art room for leisure or as a creative and enjoyable way to meet rehabilitation goals, either as an individual or as a group basis.
The purpose-built space of the OT art room has enhanced facilities and resources designed to support the complex needs of our patients. We have height-adjustable tables and adaptive equipment such as mouth painting brushes, mobile arm supports and touch screen computers. A range of activities and art forms are accessible from painting, pottery, and embroidery; we try to cater to all the wonderful ideas and creations that our patients come up with.
Art gives people a way of expressing thoughts and feelings creatively. Whatever is created in the art room can be kept by individuals as a reminder of their hard work, or shared with friends and family, promoting self-esteem and offering a sense of accomplishment.
We love to regularly celebrate and exhibit wonderful creations throughout the RHN.
Compass Assistive and Rehabilitation Technology Service
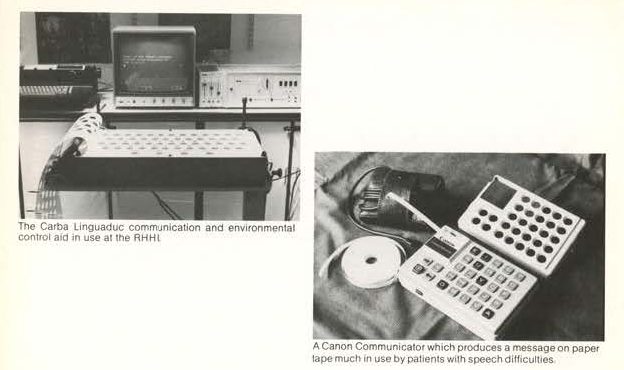
For over 30 years, the RHN has been involved in the innovative and creative use of technology to help our patients and residents. Compass was formed around 15 years ago to help progress this work as technology became more and more embedded in healthcare across many settings and technology became more complex. Part of our role is to be aware of the latest developments in technology to ensure our patients and residents have the latest equipment at their disposal. Technology moves on all the time, so it is essential to work with companies to help develop ways in which mainstream technologies can be more accessible and useful to people with disabilities.
Wheelchair services
The wheelchair department works across continuing care, specialist services and BIS at the RHN.
We make sure that all patients and residents are sitting in appropriate wheelchairs and work closely with occupational therapists and physiotherapists from across the RHN.
We have a large stock of loan wheelchairs and equipment to be able to assess users to find the best solution to meet their needs.
We also liaise with the wider network of NHS Wheelchair services to secure funding for patients’/residents’ long-term wheelchairs.
We are a small department and only have 6 permanent team members across the entire RHN